this might answer some of the ?s that've been posed---
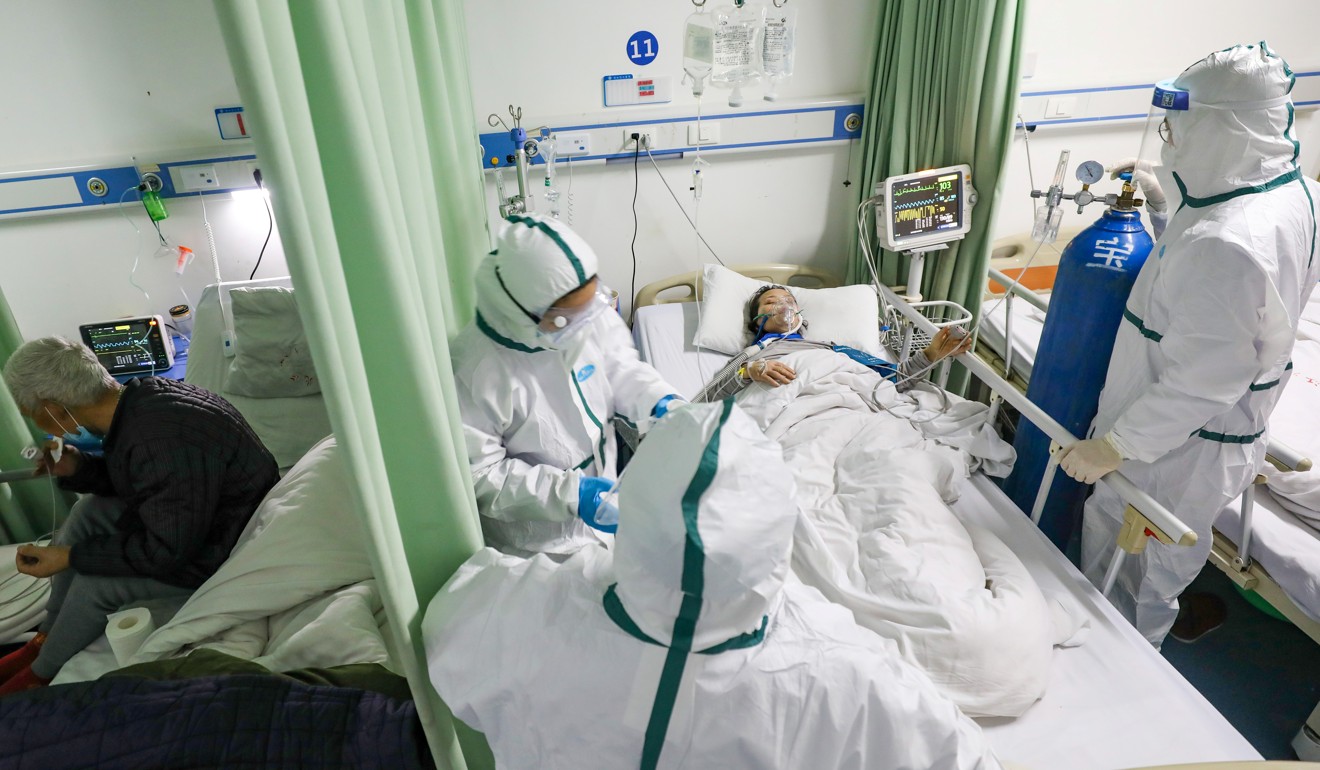
Here’s what coronavirus does to the body
From blood storms to honeycomb lungs, here’s an organ-by-organ look at how COVID-19 harms humans.
11 Minute Read
By
Amy McKeever
PUBLISHED February 14, 2020
Much remains unknown about the novel coronavirus ripping through China, but one thing is certain. The disease can cast a storm over the whole human body.
Such has been the nature of past zoonotic coronaviruses, ones that hopped from animals to humans like SARS and MERS. Unlike their common-cold-causing cousins, these emergent coronaviruses can spark a viral-induced fire throughout many of a person’s organs, and the new disease—dubbed "COVID-19" by the World Health Organization on Tuesday—is no exception when it is severe.
That helps explain why the COVID-19 epidemic has killed more than 1,300 people,
surpassing the SARS death toll in a matter of weeks. While the death rate for COVID-19 appears to be a tenth of SARS, the novel coronavirus has spread faster.
Confirmed cases
rose to more than 60,000 on Thursday, nearly a 50 percent jump relative to the prior day. This leap reflects a change in the way Chinese authorities are diagnosing infections instead of a massive shift in the scope of the outbreak. Rather than wait for patients to test positive for the virus, diagnoses
now include anyone whose chest scan reveals COVID-19’s distinctive pattern of pneumonia. This method will hopefully allow authorities to isolate and treat patients more quickly.
If this outbreak continues to spread, there’s no telling
how harmful it could become. A leading epidemiologist at the University of Hong Kong warned this week that COVID-19 could
infect 60 percent of the globe if left unchecked. On Thursday, China’s National Health Commission said
more than 1,700 health care workers are ill with the new virus, and the announcement came just a day after the
WHO wrapped a summit on the best protocols for hospital care and the development of therapeutics, like vaccines.
But what actually happens to your body when it is infected by the coronavirus? The new strain is so genetically similar to SARS that it has inherited the title
SARS-CoV-2. So combining early research on the new outbreak with
past lessons from SARS and MERS can provide an answer.
The Lungs: Ground zero
For most patients, COVID-19 begins and ends in their lungs, because like the flu, coronaviruses are respiratory diseases.
They spread typically when an infected person coughs or sneezes, spraying droplets that can transmit the virus to anyone in close contact. Coronaviruses also cause flu-like symptoms: Patients might start out with a fever and cough that progresses to pneumonia or worse. (
Find out how coronavirus spreads on a plane—and the safest place to sit).
After the SARS outbreak, the World Health Organization
reported that the disease typically attacked the lungs in three phases: viral replication, immune hyper-reactivity, and pulmonary destruction.
Not all patients went through all three phases—in fact only 25 percent of SARS patients suffered respiratory failure, the defining signature of severe cases. Likewise, COVID-19,
according to early data, causes milder symptoms in about 82 percent of cases, while the remainder are severe or critical.
Look deeper, and the novel coronavirus appears to follow other patterns of SARS, says University of Maryland School of Medicine associate professor
Matthew B. Frieman, who studies highly pathogenic coronaviruses.
In the early days of an infection, the novel coronavirus rapidly invades human lung cells. Those lung cells come in two classes: ones that make mucus and ones with hair-like batons called cilia.
Mucus, though gross when outside the body, helps protect lung tissue from pathogens and make sure your breathing organ doesn’t dry out. The cilia cells beat around the mucus, clearing out debris like pollen or viruses.
Frieman explains that SARS loved to infect and kill cilia cells, which then sloughed off and filled patients’ airways with debris and fluids, and he hypothesizes that the same is happening with the novel coronavirus. That’s because
the earliest studies on COVID-19 have shown that many patients develop pneumonia in both lungs, accompanied by symptoms like shortness of breath.
That’s when phase two and the immune system kicks in. Aroused by the presence of a viral invader, our bodies step up to fight the disease by flooding the lungs with immune cells to clear away the damage and repair the lung tissue.
When working properly, this inflammatory process is tightly regulated and confined only to infected areas. But sometimes your immune system goes haywire and those cells kill anything in their way, including your healthy tissue.
“So you get more damage instead of less from the immune response,” Frieman says. Even more debris clogs up the lungs, and pneumonia worsens. (
Find out how the novel coronavirus compares to flu, Ebola, and other major outbreaks).
Lungs 101 The lungs replenish the body with life-giving oxygen. Learn about the anatomy of the lungs, how the organs make respiration possible, and how they are vulnerable to illnesses.
During the third phase, lung damage continues to build—which can result in respiratory failure. Even if death doesn’t occur, some patients survive with permanent lung damage. According to
the WHO, SARS punched holes in the lungs, giving them “a honeycomb-like appearance”—and these lesions are present in those afflicted by
novel coronavirus, too.
These holes are likely created by the immune system’s hyperactive response, which creates scars that both protect and stiffen the lungs.
When that occurs, patients often have to be put on ventilators to assist their breathing. Meanwhile, inflammation also makes the membranes between the air sacs and blood vessels more permeable, which can fill the lungs with fluid and affect their ability to oxygenate blood.
“In severe cases, you basically flood your lungs and you can’t breathe,” Frieman says. “That’s how people are dying.”
The Stomach: A shared gateway
During the SARS and MERS outbreaks,
nearly a quarter of patients had diarrhea—a much more significant feature of those zoonotic coronaviruses. But Frieman says it’s still not clear whether gastrointestinal symptoms play a major part in the latest outbreak, given cases diarrhea and abdominal pain have been rare. But why does a respiratory virus bother the gut at all?
When any virus enters your body, it looks for human cells with its favorite doorways—proteins on the outside of the cells called receptors. If the virus finds a compatible receptor on a cell, it can invade.
What is a Virus? Scientists at USAMRID, the U.S. Army Medical Research Institute of Infectious diseases, work with some of the most deadly forms of life on earth, killer viruses. Learn more.
Some viruses are picky about which door they choose, but others are a little more promiscuous. “They can very easily penetrate into all types of cells,” says Anna Suk-Fong Lok, assistant dean for clinical research at the University of Michigan Medical School and former president of the American Association for the Study of Liver Diseases.
Both
SARS and
MERS viruses can access the cells that line your intestines and large and small colon, and those infections appear to flourish in the gut, potentially causing the damage or the leakage of fluid that becomes diarrhea.
But Frieman says we don’t know yet if the novel coronavirus does the same. Researchers
believe COVID-19 uses the same receptor as SARS, and this doorway
can be found in your lungs and small intestines.
Two studies—
one in the New England Journal of Medicine and
one preprint in medRxiv involving 1,099 cases—have also detected the virus in stool samples, which might indicate the virus could spread via feces. But this is far from conclusive.
“Whether that kind of fecal transmission is occuring for this Wuhan virus, we don’t know at all,” Frieman says. “But it definitely looks like it’s there in the stool and it looks like people do have GI symptoms associated with this.”
Blood storm
Coronaviruses can also cause problems in other systems of the body, due to the hyperactive immune response we mentioned earlier.
A
2014 study showed that 92 percent of patients with MERS had at least one manifestation of the coronavirus outside of the lungs. In fact, signs of a full body blitz have been witnessed with all three of the zoonotic coronaviruses: elevated liver enzymes, lower white blood cell and platelet count, and low blood pressure. In rare cases, patients have suffered from acute kidney injury and cardiac arrest.
But this isn’t necessarily a sign that the virus itself is spreading throughout the body, says Angela Rasmussen, a virologist and associate research scientist at Columbia University Mailman School of Public Health. It might be a cytokine storm.
Basically you’re bleeding out of your blood vessels.
Angela Rasmussen, virologist
Cytokines are proteins used by the immune system as alarm beacons—they recruit immune cells to the site of infection. The immune cells then kill off the infected tissue in a bid to save the rest of the body.
Humans rely on our immune systems to keep their cool when facing a threat. But during a runaway coronavirus infection, when the immune system dumps cytokines into the lungs without any regulation, this culling becomes a free-for-all, Rasmussen says “Instead of shooting at a target with a gun, you’re using a missile launcher,” she says. That’s where the problem arises: Your body is not just targeting the infected cells. It is attacking healthy tissue too.
The implications extend outside the lungs. Cytokine storms create inflammation that weakens blood vessels in the lungs and causes fluid to seep through to the air sacs. “Basically you’re bleeding out of your blood vessels,” Rasmussen says. The storm
spills into your circulatory system and creates systemic issues across multiple organs.
From there, things can take a sharp turn for the worse. In some of the most severe COVID-19 cases, the cytokine response—combined with a diminished capacity to pump oxygen to the rest of the body—
can result in multi-organ failure. Scientists don’t know exactly why some patients experience complications outside of the lung, but it might be linked to underlying conditions like heart disease or diabetes.
“Even if the virus doesn’t get to kidneys and liver and spleen and other things, it can have clear downstream effects on all of those processes,” Frieman says. And that’s when things can get serious.''
posted for fair use
From blood storms to honeycomb lungs, here’s an organ-by-organ look at how COVID-19 harms humans.

www.nationalgeographic.com



www.nationalgeographic.com



www.dailymail.co.uk












www.dailymail.co.uk



 Here’s what coronavirus does to the body
Here’s what coronavirus does to the body





